|
All Rights Reserved. COURSE OBJECTIVE: The purpose of this course is to educate nurses about telephone triage nursing as an expanding subspecialty and provide an overview of tools, practices, and issues common in telephone triage practice. WHAT IS TELEPHONE TRIAGE? Telephone triage is a clinical subspecialty practiced by licensed medical professionals (most frequently nurses) that involves the safe, appropriate, and timely evaluation of patient symptoms via the phone by trained clinicians. Telephone triage services can be offered within a range of practice settings, including emergency departments, general practice, primary care, pediatric practices, and managed care environments. Nursing telephone triage has become an integral mode of delivering healthcare services, especially during off- hours, on a national and international level (Huibers et al., 2. Telephone triage is defined as “an interactive process between the nurse and client that occurs over the telephone and involves identifying the nature and urgency of client healthcare needs and determining the appropriate disposition” (Rutenberg & Greenberg, 2. Telephone triage interactions may require assessment, patient education, and crisis intervention. The goal of telephone triage services is to direct the caller to the appropriate level of care or service in a safe and timely manner in combination with providing self- care advice and direction (Blank et al., 2. There are a variety of naming conventions for telephone triage services; some nurses refer to telephone triage as “telephone advice” and consider themselves advice nurses, while others use the words telepractice or telehealth. Telehealth, however, is an umbrella term that describes the delivery of healthcare services through electronic modes (Nagel et al., 2. For the purposes of this course, telephone triage is considered to be the interaction between patient and nurse that takes place exclusively by telephone. The Focus of Telephone Triage. Telephone triage is focused on the assessment and disposition of symptom- based calls rather than message taking. While message taking is a current practice in some settings, most state boards of nursing support using a professional nurse as a medical decision maker. The message- taking role is more appropriately relegated to unlicensed assistive personnel. Telephone triage does not involve making diagnoses—nursing or medical—by phone. Telenurses do not diagnose but rather collect sufficient data related to the presenting problem and medical history, recognize and match symptom patterns to those in the protocol, and assign acuity. Telenurses provide for the safe, timely disposition of health- related problems. Telephone triage aids in directing the patient to the right level of care with the right provider in the right place at the right time (Blank et al., 2. Telephone triage services can improve continuity of care, avoid unnecessary visits to the emergency room, reduce patient anxiety, provide education and self- care, and increase patient satisfaction levels as well as reduce risks from medical complications. Patients value the care that they receive. In fact, one study showed that reassurance was more important than the relief of symptoms (Wheeler, 2. Clearly, reassurance and thoughtful attention to patient concerns—whether medical, informational, or even administrative—often meet patients’ needs and provide high satisfaction. Practice Settings. 
Emergency Department Triage Julia Fuzak, MD, Patrick Mahar, MD. Nurse CEU course about telephone triage nursing. Read the course material for free. Pay for your certificate only after you pass the test! Currently, formal telephone triage is practiced in three major settings: Managed care organizations. Primary care and specialty group practices (e. Emergency departments (EDs) and crisis lines. Occasionally, telenurses encounter crisis- level calls, such as poison ingestions, domestic abuse, rape, cardiopulmonary resuscitation (CPR) coaching, or threatened suicide. However, in many communities, nonmedical personnel with specialized training operate crisis hotlines such as poison prevention, rape crisis, and suicide prevention, and customarily manage such calls. Likewise, 9. 11 medical dispatchers perform high- level telephone triage and coach callers in first- aid treatment, CPR, and the Heimlich maneuver until paramedics arrive. MANAGED CARE CALL CENTERSIn the 1. HMOs recognized telephone triage as a separate subspecialty. From that period forward, protocols, training, and standards have typically kept pace with technological advances. When high standards are maintained, telephone triage within the managed care setting is a successful, highly appreciated, and integral part of the larger system. Today, most managed care organizations as well as Medicaid use nurse telephone triage services for their members, with the goal of decreasing emergency room visits and referring to the appropriate level of care and services (Rutenberg & Greenberg, 2. Telephone triage call volume within this setting can be extremely high, making the work stressful. Attachment 9: Medical Care Triage Guidelines Contents: - Utah Pandemic Influenza Hospital and ICU Triage Guidelines for Adults - Utah Pandemic Influenza Hospital and. Evaluating EMS Field Triage Protocols and Patient Outcomes. Project Manager: Cathy Gotschall, (Email: [email protected], Phone: 202-493-0413). 
Telenurses usually have electronic algorithms or decision- support tools and access to patient demographic information via an electronic medical record (EMR) on which to rely. Typically, demographic information includes previous medications, medical history, and dates of recent medical visits. The EMR software program creates a paper trail; enables managers to track and trend calls; and creates statistics on call volume, types of calls, and individual staff workflow and dispositions. Generally, managed care call centers are larger and better organized than most small offices, group practices, and ED systems. Guidelines for the Use of. Modified Health Care Protocols in Acute Care Hospitals. During Public Health Emergencies. Originally Published November 2009. This paper examines eight publicly available critical care triage protocols intended for use during an influenza pandemic. These protocols place an emphasis on. TriageLogic myTriageChecklist Patient-Triage Assessment Form Date: AAFP Triage Protocol for Suspected Influenza Infection January 29, 2014 DISCLAIMER: This algorithm is designed only to assist physicians and those under their. In the managed- care setting, electronic protocols and algorithms are provided, as are formal training programs and standards. MEDICAL OFFICES AND EMERGENCY DEPARTMENTSOffice and ED practices can vary widely in standards and protocol availability.  
Most medical offices and specialty practices first began their triage systems using paper protocols and pen- and- paper documentation. Training may have been on- the- job. However, as the practice has evolved, basic nursing competencies in telephone triage have been established, as well as standard triage algorithms to guide nurses as they investigate patient information and symptoms (Rutenberg & Greenberg, 2. Telephone triage services that are offered within a primary care office or specialty area are meant to enhance or supplement access to care and manage appointments. This may involve reviewing test results, assisting with general healthcare questions, and assessing patient symptoms to guide the patient to the appropriate level of care. 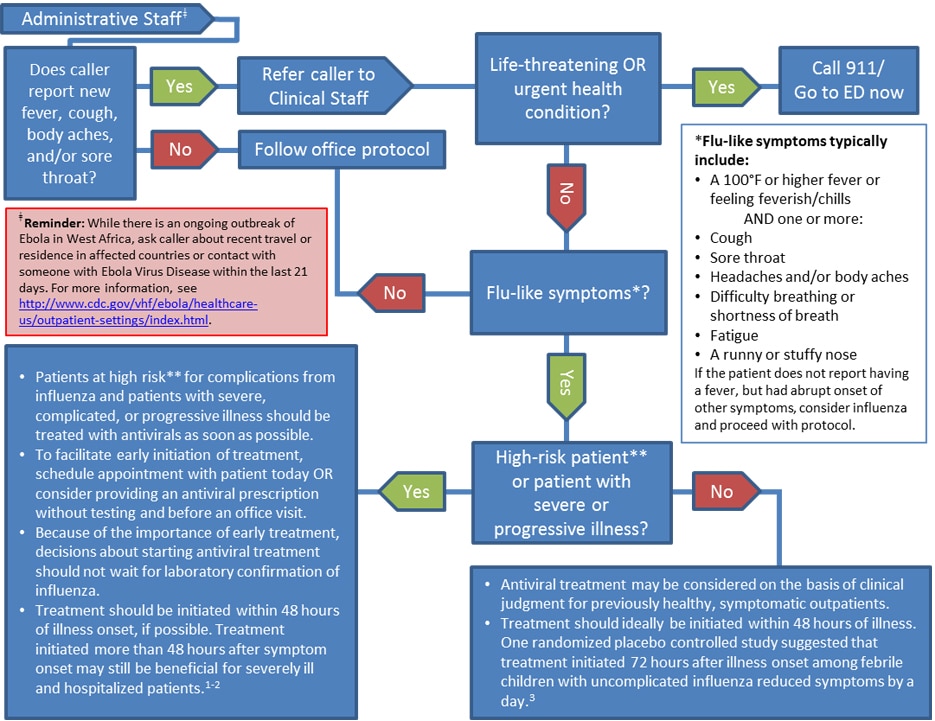
Telephone triage nurses may also make follow- up calls to high- risk patients to assess changes or check the status of symptoms after an in- person visit with the care provider (e. Telephone triage within the ED setting may involve nurses who are trained within that setting to take calls in order to determine the severity of a caller’s needs using a series of algorithms. The telephone triage process may be similar to asking questions in person as part of an intake procedure, only in this case, the patient is calling in and physical assessment and observations are not possible. The ED telephone triage nurse directs the caller to the appropriate emergency services if needed or makes recommendations for follow- up based on the established triage protocols (Rutenberg & Greenberg, 2. CRISIS LINESCrisis lines are not generally seen as providing telephone triage nursing. Obvious examples of crisis intervention lines are poison prevention, suicide prevention, rape crisis, and 9. Emergency medical dispatchers (EMDs) are nonmedical personnel or paramedics who respond to 9. They assess by phone the need for emergency service and are responsible for dispatching medical rescue vehicles to victims. Most medical dispatchers are high school graduates, two thirds are female, and most have no previous medical training. EMDs often receive some training for responding to a range of commonly encountered crisis- level medical problems. Who Are the Callers? Over the last 3. 0 years, researchers have identified predictable caller populations (e. Armed with this knowledge, staff in medical offices, managed care organizations, and emergency departments can prepare with specialized training, protocols, and staffing adequate to meet the need at predicted high- volume periods. POPULATIONSNot surprisingly, frequent callers are often from high- risk age groups: the very young, the frail elderly, and women of childbearing age. In internal medicine, women called twice as often as men. The percentage of calls made regarding children less than 4 years of age tends to be disproportionately large compared to the number of children in a given pediatric practice. CALL PATTERNSIn family practice settings, peak calling time trends fall between 1. There is also a pattern of heavy call volume Monday mornings, Friday afternoons, during the lunch hour, and in the late afternoon. This may occur as patients become aware of their own symptoms after the demands of work are finished. When calling about their children, parents may notice that their children are not well when they are reunited with them after work. In both the ED and office settings, there is a substantial volume of calls on weekends, holidays, and after hours when offices are closed and access to healthcare is limited. In a review of literature from the past decade, researchers discovered that half of all after- hours calls in a family practice occur on weekends (Huibers et al., 2. COMMON COMPLAINTSNot surprisingly, in the primary care setting a few complaints make up the bulk of calls. Most common are: Upper respiratory infections (URIs)Fever. Gastrointestinal (GI) problems. Viral infections. Minor trauma. Back pain. Anxiety. Otitis. Urinary infections. In pediatric practice settings, the majority of the calls are typically about respiratory problems, fever, GI problems, skin and infectious diseases, and trauma. In the ED setting, the top presenting problem categories are GI, respiratory, OB/GYN, and trauma (O’Malley et al., 2.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
